Severe Bursitis Of The Foot
In the foot we have a unique situation in that between the shoes that we wear and the ground that we walk on various parts of the foot are constantly being ?micro? traumatized meaning that every time we take a step we do a small amount of damage to a particular part of the foot and eventually that part of the foot begins to hurt. The body?s response to this micro-trauma is to create a bursal sac to initially protect the area but if micro-traumatized enough the bursal sac itself becomes inflamed and we have a bursitis.
Causes
Bursitis occurs when the bursae become irritated or infected, often causing pain on movement. When infection is involved, medical intervention is necessary to fight the underlying infection and prevent it from spreading, when infection is not involved, prompt medical attention can prevent the condition from becoming worse over time.
Symptoms
The main symptom of heel bursitis is pain. You may experience pain in your heel when you walk or run. There may also be pain if the area is touched or if you stand on your tiptoes. In addition to pain, the area may appear red and warm, which are both signs of inflammation. Even if you have these symptoms, only a doctor can determine if you have bursitis of the heel. Your doctor will use these symptoms along with a general exam to determine if you are suffering from bursitis of the heel.
Diagnosis
Obtaining a detailed history from the patient is important in diagnosing calcaneal bursitis. The following complaints (which the physician should ask about during the subjective examination) are commonly reported by patients.
Other inquiries that the physician should make include the following. The clinician should ask about the patient's customary footwear (whether, for example, it includes high-heeled shoes or tight-fitting athletic shoes). The patient should be asked specifically about any recent change in footwear, such as whether he/she is wearing new athletic shoes or whether the patient has made a transition from flat shoes to high heels or vice versa. Individuals who have been accustomed to wearing high-heeled shoes on a long-term basis may find that switching to flat shoes causes increased stretch and irritation of the Achilles tendon and the associated bursae. The specifics of a patient's activity level should be ascertained, including how far the patient runs and, in particular, whether the individual is running with greater intensity than before or has increased the distance being run. The history of any known or suspected underlying rheumatologic conditions, such as gout, rheumatoid arthritis, or seronegative spondyloarthropathies, should be obtained.
Non Surgical Treatment
Long Term Treatment must be directed towards eliminating the abnormal tilting of the heel, regardless of its cause. If this is delayed, the usual results are the pain and swelling becomes worse, chronic, and debilitating. Eventually, painful calcifications and bone spur formations may occur on the back of the heel, along with tears in the Achilles Tendon. These are serious problems that may require surgical intervention. In order to eliminate abnormal heel tilt, the foot must be re-balanced. Controlling and reducing the biomechanical foot defects that are causing the heel to tilt best accomplish this. The "Gold Standard" of medical care (that treatment most used by doctors and therapists) to help eliminate pain, inflammation, and swelling at the back of the heel is orthotics.
Surgical Treatment
Bursectomy is a surgical procedure used to remove an inflamed or infected bursa, which is a fluid-filled sac that reduces friction between tissues of the body. Because retrocalcaneal bursitis can cause chronic inflammation, pain and discomfort, bursectomy may be used as a treatment for the condition when it is persistent and cannot be relived with other treatments. During this procedure, a surgeon makes small incisions so that a camera may be inserted into the joint. This camera is called an arthroscope. Another small incision is made so that surgical instruments can be inserted to remove the inflamed bursa.
Prevention
Continue to wear your orthotics for work and exercise to provide stability and restore foot function. Select suitable shoes for work and physical activity that provide stability for the heel. Regular stretching of the calf muscle can prevent heel bursitis. Do not suddenly increase activity amount without appropriate conditioning.
Hammer Toe Operation And Recovery
The hammertoe condition is usually irreversible, but often its progression can be slowed or halted. You should visit a Podiatrist if the toe becomes painful and you have difficulty walking. A Podiatrist will be able to provide advice and treatment including padding the bony top-part of your hammertoe to relieve pain or to tape your toes as a way to change their position. Podiatrists have an important role to play in preventing and managing foot problems. Prompt action is important. Problems which are left without assessment or treatment may result in major health risks.
Causes
A hammertoe is formed due an abnormal balance of the muscles in the toes. This abnormal balance causes increased pressures on the tendons and joints of the toe, leading to its contracture. Heredity and trauma can also lead to the formation of a hammertoe. Arthritis is another factor, because the balance around the toe in people with arthritis is so disrupted that a hammertoe may develop. Wearing shoes that are too tight and cause the toes to squeeze can also be a cause for a hammertoe to form.
 Symptoms
Symptoms
At first, a hammertoe or mallet toe may maintain its flexibility and lie flat when you're not wearing crowded footwear. But eventually, the tendons of the toe may contract and tighten, causing your toe to become permanently stiff. Your shoes can rub against the raised portion of the toe or toes, causing painful corns or calluses.
Diagnosis
Your healthcare provider will examine your foot, checking for redness, swelling, corns, and calluses. Your provider will also Hammer toe measure the flexibility of your toes and test how much feeling you have in your toes. You may have blood tests to check for arthritis, diabetes, and infection.
Non Surgical Treatment
There is a variety of treatment options for hammertoe. The treatment your foot and ankle surgeon selects will depend upon the severity of your hammertoe and other factors. A number of non-surgical measures can be undertaken. Padding corns and calluses. Your foot and ankle surgeon can provide or prescribe pads designed to shield corns from irritation. If you want to try over-the-counter pads, avoid the medicated types. Medicated pads are generally not recommended because they may contain a small amount of acid that can be harmful. Consult your surgeon about this option. Changes in shoewear. Avoid shoes with pointed toes, shoes that are too short, or shoes with high heels, conditions that can force your toe against the front of the shoe. Instead, choose comfortable shoes with a deep, roomy toe box and heels no higher than two inches. Orthotic devices. A custom orthotic device placed in your shoe may help control the muscle/tendon imbalance. Injection therapy. Corticosteroid injections are sometimes used to ease pain and inflammation caused by hammertoe. Medications. Oral nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be recommended to reduce pain and inflammation. Splinting/strapping. Splints or small straps may be applied by the surgeon to realign the bent toe.
Surgical Treatment
If your toe is not bendable, your doctor may recommend surgery. The type of surgery that will be performed will depend on the severity of the condition. You should expect blood and urine studies before the procedure, as well as x-rays of your feet. Your doctor will inject either a local or regional anesthetic. If your toe has some flexibility, the doctor may be able to straighten it by simply making an incision in the toe to release or lengthen the tendon. If the toe is not flexible, your doctor will probably make the same incision to release the tendon, but he or she may also remove some pieces of the bone so that the bone can be straightened. A k-wire is placed in the toe to help hold it straight while it is healing. This is taken out after about four weeks.
Hammer Toe Causes And Treatments
 Overview
Overview
A hammertoe is a term used to describe a crooked, deviated, or contracted toe. Although the condition usually stems from muscle imbalance, it is often aggravated by poor-fitting shoes or socks that cramp the toes. Over a period of years, the tendons that move the toe up and down begin to pull the toe with unequal tension, and the toe then begins to buckle or become contracted, causing an abnormal "v"-shaped bending of the little toes. Patients with this condition often experience pain, swelling, redness and stiffness in the affected toes.
Causes
People who are born with long bones in their toes are more likely to develop hammer toe. Children who wear shoes they have outgrown may develop this Hammer toe condition. People who wear very narrow shoes or high-heeled shoes are also more likely to develop a hammer toe. Sometimes, pressure from a bunion can cause hammer toe. Rheumatoid arthritis is another a risk factor.
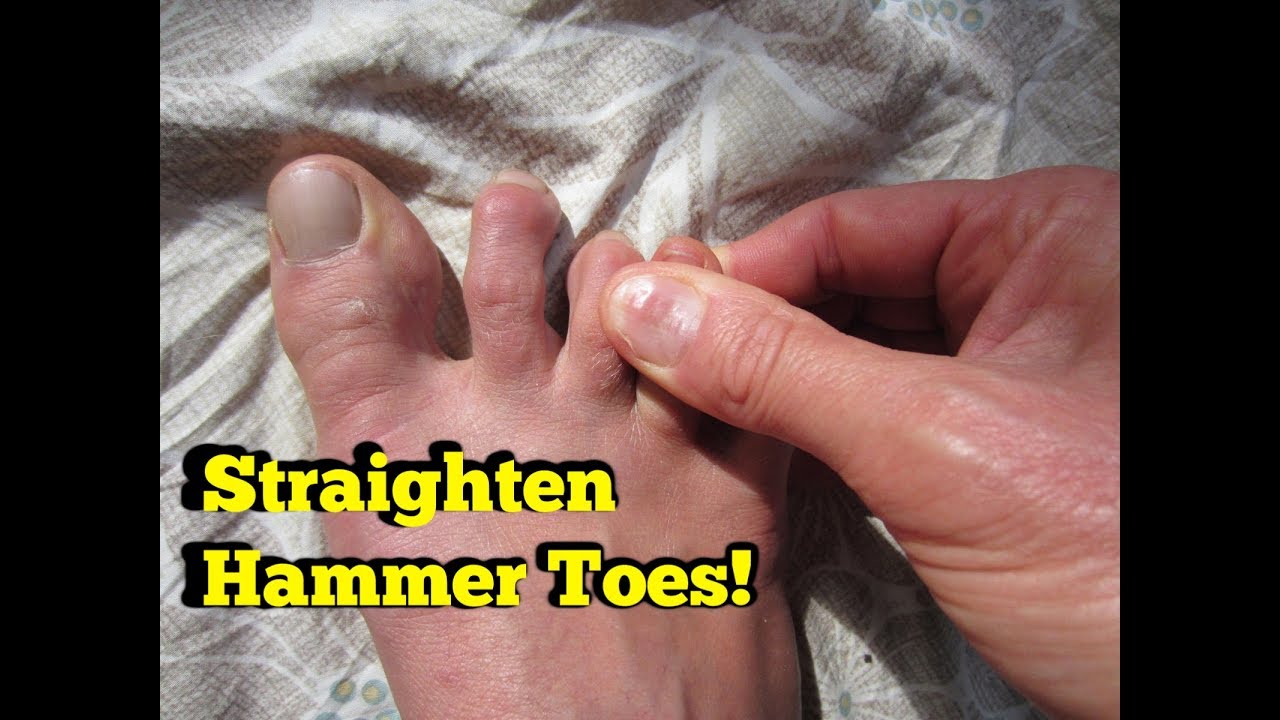 Symptoms
Symptoms
Hammer toe is often distinguished by a toe stuck in an upside-down ?V? position, and common symptoms include corns on the top of your toe joint. Pain at the top of a bent toe when you put on your shoes. Pain when moving a toe joint. Pain on the ball of your foot under the bent toe. Corns developing on the top of the toe joint. It is advisable to seek medical advice if your feet hurt on a regular basis. It is imperative to act fast and seek the care of a podiatrist or foot surgeon. By acting quickly, you can prevent your problem from getting worse.
Diagnosis
The treatment options vary with the type and severity of each hammer toe, although identifying the deformity early in its development is important to avoid surgery. Your podiatric physician will examine and X-ray the affected area and recommend a treatment plan specific to your condition.
Non Surgical Treatment
Prescription strength medicines to decrease pain and inflammation. Physical Therapy. To strengthen poorly functioning muscles and stretch tight muscles that may be exacerbating the toes. Special ultrasound techniques may reduce inflammation. Custom Foot Orthotics. An orthotic with an exact mold of your foot to better align and support the foot to ease current discomfort and prevent future progression. Toe Splints or Pads. Specific pads may prevent pressure and physical irritation in shoes. Toe splints and toe spacers physically realign the toes and can lessen pain and halt or stall hammer toe progression. Cortisone injections are strong anti-inflammatory agents to decrease pain, and swelling directly at the toe region. Injections only treat the symptoms, and in some cases used in caution (and sparingly) they can weaken supporting ligaments of the toe(s).
Surgical Treatment
If conservative treatments don't help, your doctor may recommend surgery to release the tendon that's preventing your toe from lying flat. In some cases, your doctor might also remove some pieces of bone to straighten your toe.
Are Bunions And Corns The Same Thing
Overview
 Sometimes, the big toe can become angled outwards towards the middle of the foot and second toe. This forces the top of the first metatarsal to stick out from the side of the foot at the base of the big toe. If this happens, the bones can become misaligned and a painful bunion can form. It is not known exactly what causes bunions, but wearing badly fitting shoes is thought to make the condition worse. Research also suggests that bunions may run in families. It is thought that bunions are more likely to occur in people who have unusually flexible joints, and that this flexibility may be inherited. In some cases, certain health conditions, such as rheumatoid arthritis and gout, may also be responsible for the formation of bunions. These conditions cause pain and inflammation in the joints.
Sometimes, the big toe can become angled outwards towards the middle of the foot and second toe. This forces the top of the first metatarsal to stick out from the side of the foot at the base of the big toe. If this happens, the bones can become misaligned and a painful bunion can form. It is not known exactly what causes bunions, but wearing badly fitting shoes is thought to make the condition worse. Research also suggests that bunions may run in families. It is thought that bunions are more likely to occur in people who have unusually flexible joints, and that this flexibility may be inherited. In some cases, certain health conditions, such as rheumatoid arthritis and gout, may also be responsible for the formation of bunions. These conditions cause pain and inflammation in the joints.
Causes
There is no single cause of hallux valgus. It most commonly runs in families but may skip generations. High heel, pointed toe shoes are not the primary cause of the hallux valgus but they do cause it to be painful. Pressure from shoes may cause bunions, corns and calluses to develop where there is hallux valgus deformity.
Symptoms
The most obvious symptoms of a bunion are. Pain in the area of the MTP joint, the joint where your big toe connects to your foot. Bending of the big toe in towards the other toes. An enlarged bump of bone or tissue at the MTP joint. Each symptom can range in degree from small to severe. Sometimes the pain can be sufficient to make it difficult to walk in normal shoes. Other symptoms may include. Swelling and inflammation of the skin around the MTP joint. Thickening of the skin in the area of the joint. Restricted motion in your big toe. Pressure from the inward bending of your big toe can affect your other toes, leading to corns on your smaller toes. Ingrown toenails on the smaller toes. Development of hammertoes in the other toes. Calluses on the bottom of your foot. If you have any of these symptoms, especially pain, displacement of your big toe or development of a bulge, you should consider consulting your physician. Even if you're not significantly bothered by some of these symptoms, bunions tend to continue getting bigger and more serious over time and should be taken care of before they do so.
Diagnosis
Before examining your foot, the doctor will ask you about the types of shoes you wear and how often you wear them. He or she also will ask if anyone else in your family has had bunions or if you have had any previous injury to the foot. In most cases, your doctor can diagnose a bunion just by examining your foot. During this exam, you will be asked to move your big toe up and down to see if you can move it as much as you should be able to. The doctor also will look for signs of redness and swelling and ask if the area is painful. Your doctor may want to order X-rays of the foot to check for other causes of pain, to determine whether there is significant arthritis and to see if the bones are aligned properly.
Non Surgical Treatment
Bunion treatment should always start with changing footwear to relieve symptoms and to prevent the bunion from progressing. Shoes with a wide toe-box, minimal slope, and good arch support can help relieve the bunion pain. Some people find that ice application and anti-inflammatory medications can help relieve the inflammation around the bunion. 
Surgical Treatment
If conservative treatment doesn't provide relief from your symptoms, you may need surgery. The goal of bunion surgery is to relieve discomfort by returning your toe to the correct position. There are a number of surgical procedures for bunions, and no one technique is best for every problem. Surgical procedures for bunions might involve removing the swollen tissue from around your big toe joint. Straightening your big toe by removing part of the bone. Realigning the long bone between the back part of your foot and your big toe, to straighten out the abnormal angle in your big toe joint. Joining the bones of your affected joint permanently. It's possible you may be able to walk on your foot immediately after a bunion procedure. However, full recovery can take weeks to months. To prevent a recurrence, you'll need to wear proper shoes after recovery. It's unlikely that you'll be able to wear narrower shoes after surgery. Surgery isn't recommended unless a bunion causes you frequent pain or interferes with your daily activities. Talk to your doctor about what you can expect after bunion surgery.
Prevention
Make better shoe choices. If you?re a woman, avoid high-heeled footwear whenever possible (at the very least, choose shoes with heels lower than two inches), and make sure all your footwear has a wide, deep toe box. Whether man or woman, if you?re trying on shoes and your toes feel ?squished? or crowded by a particular shoe, reject that style and try another, or go for a larger size. You don?t need to invite trouble. In general, shoes that come to a point at the toe are bad news, as they tend to push the toes together into an overlapping pattern. Shoes with rocker soles will unload pressure on the bunion area. Examine your feet regularly. Note any redness, swelling or discoloration. Flex your toes and check for any stiffness. If there is any, think back to what you?ve worn or done in the past few days. If the condition persists more than a few days, or worsens, a visit to the podiatric physician is in order.
How Do I Know If I Have Overpronation
Overpronation is by far the most common foot type. Pronation is not linked one-to-one with low arches. Although pronation lowers the arches, this does not mean that only those with low arches overpronate. People with high arches can also overpronate! Some of us have always overpronated, for others overpronation develops with age, weight gain, regular standing work or intensive exercise. Pronounced wear on the instep side of shoe heels can indicate overpronation, however it's best to get an accurate assessment.

Causes
You do not have to be a runner or athlete to suffer from overpronation. Flat feet can be inherited, and many people suffer from pain on a day-to-day basis. Flat feet can also be traumatic in nature and result from tendon damage over time. Wearing shoes that do not offer enough arch support can also contribute to overpronation.
Symptoms
Eventually, over-pronation can lead to a full list of maladies including flat feet, plantar fasciitis, plantar fibroma, neuromas, heel spurs, shin splints, ankle sprains, bunions, hammertoes, calluses, and pain in the arches, knee, hip and lower back. But it doesn?t have to go that far, because there are steps we can take to correct the over-pronation. In the vast majority of cases, we?ll prescribe custom foot orthotics, which will realign your ankles, redistribute the weight, support the arch and reduce the twisting. Many orthotics will fit snugly into your normal shoes. Although we?ll also take a look at the type of shoes you wear to see if they are contributing to the problem.
Diagnosis
Bunions, calluses and crooked toes may indicate alignment problems. So, it is important to ascertain the condition of a client's toes. Check the big toe to determine if the first joint of the toe is swollen, has a callus or bunion, and/or looks as though it abducts (i.e., hallux valgus) rather than pointing straight ahead. Also, look to see if the lesser toes seem to "curl up" (i.e., the person has hammer or claw toes). This may be indicative of damage to, or inflexibility of the plantar fascia caused by excessive flattening of the foot.

Non Surgical Treatment
Orthotics are medical devices used to provide support to correct a physical abnormality. They can provide arch support when needed to remedy over-pronation, and in this particular cases the orthoses used are usually convenient shoe inserts. These can be taken in and out of shoes, and will be carefully tailored by your podiatrist to the specifics of your foot. It can take some weeks before the effects of the inserts can become truly noticeable, and in many cases your podiatrist will want to review your orthotics within a few weeks to make fine adjustments based on how well they have worked to reduce your pain.
Prevention
Custom-made orthotics supports not only the arch as a whole, but also each individual bone and joint that forms the arch. It is not enough to use an over-the-counter arch support, as these generic devices will not provide the proper support to each specific structure of the arch and foot. Each pronated foot?s arch collapses differently and to different degrees. The only way to provide the support that you may need is with a custom-made device. This action of the custom-made orthotic will help to prevent heel spurs, plantar fasciitis, calluses, arch pain, and weakness of the entire foot.
Ways To Treat Calcaneal Apophysitis?
Sever's Disease is one of the most common causes of heel pain in active adolescents. Hip stability is restored using a non-surgical positioning device. Symptoms of Sever's disease are relieved through a combination of conservative treatment options and preventative measures can be taken to decrease the risk of developing the condition.
Causes
When a baby is born, most of the bones are still cartilage with only some starting to develop into bone. When the heel (calcaneus) starts to develop bone, there is generally one large area of development that starts in the center of the cartilage heel. This area of bone spreads to 'fill up' the cartilage. Another area of bone development (ossification) occurs at the back of the heel bone. These two areas of developing bone will have an area of cartilage between them, this is how the bone grows in size. At around age 16, when growth is nearly complete, these two bony areas fuse together. Sever's disease or calcaneal apophysitis is usually considered to be due to damage or a disturbance in this area of growth.
Symptoms
The most obvious sign of Sever's disease is pain or tenderness in one or both heels, usually at the back. The pain also might extend to the sides and bottom of the heel, ending near the arch of the foot. A child also may have these related problems, swelling and redness in the heel, difficulty walking, discomfort or stiffness in the feet upon awaking, discomfort when the heel is squeezed on both sides, an unusual walk, such as walking with a limp or on tiptoes to avoid putting pressure on the heel. Symptoms are usually worse during or after activity and get better with rest.
Diagnosis
To diagnose the cause of the child?s heel pain and rule out other more serious conditions, the foot and ankle surgeon obtains a thorough medical history and asks questions about recent activities. The surgeon will also examine the child?s foot and leg. X-rays are often used to evaluate the condition. Other advanced imaging studies and laboratory tests may also be ordered.
Non Surgical Treatment
The treatment of Sever's disease depends upon the severity of symptoms experienced by the patient. Care is initiated with a simple program of stretching and heel elevation to weaken the force applied to the calcaneus by the Achilles tendon. If stretches and heel elevation are unsuccessful in controlling the symptoms of Sever's disease, children should be removed from sports and placed on restricted activities. Mild Symptoms. Wear a 3/8 heel lift at all times (not just during physical activity). It is important to use a firm lift and not a soft heel pad. Calf stretches 6/day for 60 seconds each. Calf stretches are best accomplished by standing with the toes on the edge of a stretching block. Moderate Symptoms. Follow the directions for minor symptoms and decrease activity including elimination of any athletic activity. In addition to stretching by day, a night stretching splint can be worn while sleeping. Severe Symptoms. Follow the directions for mild and moderate symptoms. Children should be removed from sports activities such as football, basketball, soccer or gym class. A below knee walking cast with a heel lift or in severe cases, non-weight bearing fiberglass cast, may be indicated for 4-6 weeks. The cast should be applied in a mildly plantar flexed position. Cam Walkers should not be used for Sever's Disease unless they have a built in heel lift.
Flat Feet In Adults
Overview
The posterior tibial tendon serves as one of the major supporting structures of the foot, helping it to function while walking. Posterior tibial tendon dysfunction (PTTD) is a condition caused by changes in the tendon, impairing its ability to support the arch. This results in flattening of the foot. PTTD is often called ?adult acquired flatfoot? because it is the most common type of flatfoot developed during adulthood. Although this condition typically occurs in only one foot, some people may develop it in both feet. PTTD is usually progressive, which means it will keep getting worse, especially if it isn?t treated early. 
Causes
The most common cause of acquired adult flatfoot is posterior tibial tendon dysfunction. What causes adult acquired flat foot? Fracture or dislocation. Tendon laceration. Tarsal Coalition. Arthritis. Neuroarthropathy. Neurological weakness.
Symptoms
The first stage represents inflammation and symptoms originating from an irritated posterior tibial tendon, which is still functional. Stage two is characterized by a change in the alignment of the foot noted on observation while standing (see above photos). The deformity is supple meaning the foot is freely movable and a ?normal? position can be restored by the examiner. Stage two is also associated with the inability to perform a single-leg heel rise. The third stage is dysfunction of the posterior tibial tendon is a flatfoot deformity that becomes stiff because of arthritis. Prolonged deformity causes irritation to the involved joints resulting in arthritis. The fourth phase is a flatfoot deformity either supple (stage two) or stiff (stage 3) with involvement of the ankle joint. This occurs when the deltoid ligament, the major supporting structure on the inside of the ankle, fails to provide support. The ankle becomes unstable and will demonstrate a tilted appearance on X-ray. Failure of the deltoid ligament results from an inward displacement of the weight bearing forces. When prolonged, this change can lead to ankle arthritis. The vast majority of patients with acquired adult flatfoot deformity are stage 2 by the time they seek treatment from a physician.
Diagnosis
Observation by a skilled foot clinician and a hands-on evaluation of the foot and ankle is the most accurate diagnostic technique. Your Dallas foot doctor may have you do a walking examination (the most reliable way to check for the deformity). During walking, the affected foot appears more pronated and deformed. Your podiatrist may do muscle testing to look for strength deficiencies. During a single foot raise test, the foot doctor will ask you to rise up on the tip of your toes while keeping your unaffected foot off the ground. If your posterior tendon has been attenuated or ruptured, you will be unable to lift your heel off the floor. In less severe cases, it is possible to rise onto your toes, but your heel will not invert normally. X-rays are not always helpful as a diagnostic tool for Adult Flatfoot because both feet will generally demonstrate a deformity. MRI (magnetic resonance imaging) may show tendon injury and inflammation, but can?t always be relied on for a complete diagnosis. In most cases, a MRI is not necessary to diagnose a posterior tibial tendon injury. An ultrasound may also be used to confirm the deformity, but is usually not required for an initial diagnosis.
Non surgical Treatment
Nonoperative treatment of posterior tibial tendon dysfunction can be successful with the Arizona AFO brace, particularly when treatment is initiated in the early stages of the disease. This mandates that the orthopedist has a high index of suspicion when evaluating patients to make an accurate diagnosis. Although there is a role for surgical management of acquired flat feet, a well-fitted, custom-molded leather and polypropylene orthosis can be effective at relieving symptoms and either obviating or delaying any surgical intervention. In today's climate of patient satisfaction directed health care, a less invasive treatment modality that relieves pain may prove to be more valuable than similar pain relief that is obtained after surgery. Questions regarding the long-term results of bracing remain unanswered. Future studies are needed to determine if disease progression and arthrosis occur despite symptomatic relief with a brace. Furthermore, age- and disease stage-matched control groups who are randomized to undergo surgery or bracing are necessary to compare these different treatment modalities. 
Surgical Treatment
In cases of PTTD that have progressed substantially or have failed to improve with non-surgical treatment, surgery may be required. For some advanced cases, surgery may be the only option. Surgical treatment may include repairing the tendon, tendon transfers, realigning the bones of the foot, joint fusions, or both. Dr. Piccarelli will determine the best approach for your specific case. A variety of surgical techniques is available to correct flexible flatfoot. Your case may require one procedure or a combination of procedures. All of these surgical techniques are aimed at relieving the symptoms and improving foot function. Among these procedures are tendon transfers or tendon lengthening procedures, realignment of one or more bones, or insertion of implant devices. Whether you have flexible flatfoot or PTTD, to select the procedure or combination of procedures for your particular case, Dr. Piccarelli will take into consideration the extent of your deformity based on the x-ray findings, your age, your activity level, and other factors. The length of the recovery period will vary, depending on the procedure or procedures performed.